|
|||||||||||||||||||||
|
|
|||||||||||||||||||||
|
Global Standardization Activities Vol. 9, No. 4, pp. 57–62, Apr. 2011. https://doi.org/10.53829/ntr201104gls Trends, Standardization, and Interoperability of Healthcare InformationAbstractThis article introduces formats for storing medical and healthcare information, their advantages, the ways in which they are approached in Japan and overseas, and trends for ensuring standardization and interoperability.
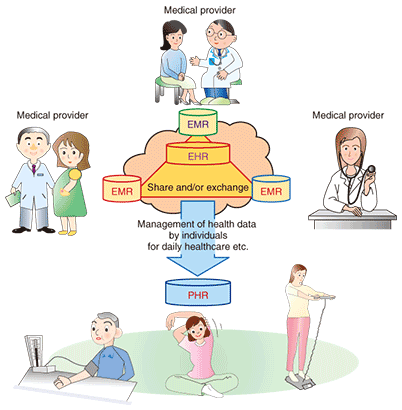
1. IntroductionVarious systems are currently being implemented to take advantage of information and communications technologies (ICT) to effectively and efficiently store and utilize medical and healthcare information, which is usually stored in a dispersed manner. The purpose is to address social challenges in the medical and health fields, as typified by soaring medical expenses. In this article, I introduce formats for storing medical and healthcare information, their advantages, the ways in which they are approached in Japan and overseas, and trends for ensuring standardization and interoperability. 2. Storage formatsInformation related to medical and health matters covers a wide range, from that with a direct relationship with medical care, such as checkup results and prescriptions, to client management, accounting, and requests for medical care repayment. This article treats the electronic storage of records related to the medical and healthcare concerns of individual patients. There are three main types of medical and healthcare information: electronic medical records (EMRs), electronic health records (EHRs), and personal health records (PHRs). EMRs are medical and health records shared within a medical organization; EHRs are ones shared among several medical organizations, such as through cooperation within a region; and PHRs are ones managed by individuals themselves (Fig. 1).
3. Definitions of EMR, EHR, and PHRDetailed definitions for EMR, EHR, and PHR have not yet been fixed. According to a report related to the definitions of medical information technology (IT) terminology written by the USA’s National Alliance for Health Information Technology (NAHIT) in April 2008 [1], there are many definitions in existence: 35 for EMR, 99 for EHR, and 52 for PHR, as listed in Table 1. Excluding definitions that have duplicate contents, the numbers of unique definitions are 26, 63, and 36, respectively. Thus, if it is not yet possible to achieve a consensus on definitions, we have a situation in which opinions among specialists are divided. New, integrated definitions of these terms proposed by NAHIT in that report are given in Table 2.
4. Advantages of implementationThe advantages of implementing EMRs, EHRs, and PHRs differ for each type of record (see Fig. 2). Recording patients’ medical care information electronically as EMRs within a medical organization enables that information to be collected and utilized within that medical organization. It also reduces the dangers of paper dust and misreading of records that occurs with paper cards, so we can expect it to lead to greater medical safety.
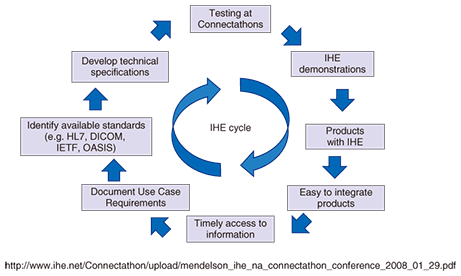
In addition, along with the process of converting records to electronic form as EMRs, EHRs can be implemented by connections via networks to outside medical organizations. Once EHRs have been implemented regionally or nationally, patients’ medical care information can be shared among medical organizations, enabling seamless medical continuity by access to the same medical care information even when, for example, patients transfer to other hospitals. In addition, by eliminating duplicate examinations and misdiagnoses at an early stage, this system can be expected to lead to more efficient medical fees and increased medical safety. The use of PHRs to enable individuals to manage and make use of their own medical and healthcare information recorded in EMRs and EHRs should lead to improvements in general health consciousness and comprehension, avert adult-onset diseases, and prevent any worsening of existing conditions. Furthermore, these records can be used for second opinions and other medical care as the individual patients wish, so various improvements, such as improvements in the quality of medical care, including emergency care, and reductions in unnecessary procedures can be expected. Below, I give an overview of trends for EHRs and PHRs, which can be expected to contribute to the medical and health fields in the future through the use of networks and which are currently being reviewed and configured both in Japan and overseas. 5. Overseas trends for EHRs and PHRsOver the past ten years or so, various EHR and PHR systems have been constructed in developed economies overseas, mainly as the result of national policies. In 2002, the UK’s National Health Service started a ten-year project called “Connecting for Health” [2], which is intended to implement a mechanism for sharing records that have been converted into electronic form. In addition to enabling the sharing of patient information summaries online, various other functions are in operation such as electronic management of prescriptions, medical appointment services, effective secondary utilization of data, email, medical service analysis systems, and a newborn registration system. The Canadian Infoway system has been set up to ensure that much of the work of confirming consultation history, checkup results, medication history, and medical images within the country can be done by means of EHRs. In the USA, the Bush administration set up an initiative with the objective of “EHR for All Americans by 2014” in April 2004. It has been handed over to the current Obama administration. The American Recovery and Reinvestment Act of 2009 [3], which was approved in February 2009, ensures various budgets, such as US$2 billion for government-affiliated medical IT promotions and US$20.8 billion for incentives to introduce medical IT systems. These measures are forecast to improve medical safety and quality through the sharing and utilization of information both within and among medical organizations, and hence reduce the public’s medical expenses. There are also procedures under way at the moment to provide subsidies for the meaningful use of such data. Similarly, initiatives related to EHRs and PHRs are also in progress in the Asian and Oceanic regions in various places from Australia and New Zealand to China, South Korea, Taiwan, and Singapore. 6. Domestic trends for EHRs and PHRsWithin Japan, businesses that utilize ICT in the medical and health fields have been doing so for some time, but the debate into the proactive utilization of networks that would enable EHRs and PHRs started in earnest in 2007 with the Ministry of Health, Labour, and Welfare’s (MHLW’s) Grant-in-Aid for Creative Scientific Research “Research Aimed at Implementing Japanese-version EHRs” and the Ministry of Economy, Trade, and Industry’s (METI’s) “Research into New Health Service Utilizing Japanese-version PHRs”. In 2008, a three-year project entitled “Healthcare Information Utilization Foundation Demonstration” was initiated through cooperation between the Ministry of Internal Affairs and Communications, MHLW, and METI, and examination of actual operations for EHRs and PHRs is well under way. In addition, in June 2010, the Japanese government’s IT Strategic Headquarters published the “New Information Communications Technology Strategy Schedule” [4], which describes the initiative called “My Hospital Everywhere (Japanese Personal Health Record)” and seamless regional healthcare enterprises, which are closely linked to the use of EHRs and PHRs. At present, specific reviews into what kind of system the IT Strategic Headquarters should implement in accordance with this schedule are under way. 7. Standardization activities related to EHRs and PHRsStandardization is important in order to enable the use of networks to share and utilize medical and healthcare information. Information related to medical and health matters comes in many different forms; in addition to the names of diseases, drugs, and treatments, there is also other data such as images, numerical values of examination results, graphs, and text. Furthermore, to ensure the connection of different systems among institutions, regions, and nations, it is necessary to integrate details such as terminology, encoding, protocol, and security. Standardization is also likely to play an extremely large role in facilitating long-term storage. At the moment, there are many standardization organizations, such as the International Organization for Standardization (ISO) and the Comité Européen de Normalisation (CEN). They are all actively working towards the standardization of both EHRs and PHRs. Below, I introduce some representative examples of these activities [5]. Health Level Seven (HL7) is a standards agreement for the exchange of medical information, such as measurement data and text, that was established in the USA in 1987. In Japan, the HL7 Japan branch was established in 1998 and is still currently active. The name HL7 comes from the seventh level (application level) of the communications model for Open System Interconnection (OSI), which is ISO’s communications specifications. These specifications lay out details such as data definitions, the timings of information exchange, and application error processing. The Japan Industrial Association of Radiological Systems [6] has been tackling standardization and legislative problems in the field of radiological sciences since its establishment in 1924. In particular, the Digital Imaging and Communication in Medicine commission has been set up within the Medical Imaging Systems Committee to develop, spread, and promote standards specifications that have defined the formats and communications protocols for medical images captured by devices such as magnetic resonance imaging and computed tomography equipment. The Japanese Association of Healthcare Information Systems Industry is conducting investigative research and promotion related to improving the relevant technology and ensuring both quality and safety. It is also conducting activities related to participation, policies, and institutions from a technological viewpoint for standardization and promotion. The Continua Health Alliance [7] was established with the objective of digitizing health-related and medical equipment and integrating communications specifications to improve the quality of health management of individuals, and over 230 businesses worldwide have become members, including 40 within Japan. Health-related and other equipment developed by member companies is developed in accordance with Continua’s design guidelines. Continua-compliant approval ensures that health-related equipment for the home, such as blood-pressure monitors and weighing machines, and medical equipment used in medical organizations can work together seamlessly with these systems and services. In this manner, standardization activities are progressing in various different organizations. In Japan, the Health Information and Communication Standards Board (HELICS) holds talks concerning the details and directions of standardization with the aim of implementing consistent activities among organizations working to standardize healthcare and welfare information. HELICS conferences do not implement standardization themselves: they review the standards specifications of Japanese standardization bodies and issue recommendations to MHLW as medical information standardization guidelines. MHLW provides a forum for discussing specifications that ought to be accepted as standards specifications in the healthcare information field at the Healthcare Information Standardization Conference. On March 31, 2010, it set out eight standards specifications as MHLW Standards Specifications [8]. Their implementation is not compulsory by law, but considering the advantages of complying with the standards, measures based on MHLW Standards Specifications will be specified in various requirement and subsidiary businesses related to medical information systems implemented in MHLW in the future. 8. Ensuring interoperabilityAs we have shown in this overview, there are various different standards specifications in existence, but even if they are followed, there will often be interoperability problems in practice when actual products are connected. The initiative for Integrating the Healthcare Enterprise (IHE) is working to resolve such problems. In 1998, IHE started operation in collaboration with the Radiological Society of North America (RSNA) and the Healthcare Information and Management Systems Society (HIMSS), and it has since expanded internationally. Japan joined in 2001 and has recently become more active. IHE clarifies how standards specifications should be applied for information exchange by setting up a workflow for each sequence of actions, such as from the issue of a request for a checkup to receipt of the results. This ensures interoperability that is even easier to implement. This workflow, which is called an integration profile, is laid out in a document called an IHE technological framework. IHE also conducts a connection test called a Connectathon (a portmanteau word combining connect and marathon) and is active in providing information about connectivity by publishing the results of this test. The cycle of IHE activities, including the above, is shown in Fig. 3. [9]. Medical organizations that have IT-related problems, such as interoperability ones, are implementing information systems that can operate with other systems, even with types of medical equipment and equipment from other vendors, by using IHE to draw up an integrated profile and technological framework, implementing them in workshops and products through the vendors, and then selecting a vendor on the basis of an integrated statement that summarizes the Connectathon results and the IHE response.
9. Future directionsIn the past, Western countries have enthusiastically promoted EHR and PHR structures, and in Japan, the “My Hospital Everywhere (Japanese Personal Health Record)” initiative and regional healthcare enterprises are progressing steadily, mainly due to government initiatives. More specifically, standard documentation formats are being maintained for purposes ranging from medical care statements and dispensing information to medical checkup information, hospital discharge summaries for the patients themselves (hospitalization record summaries), and checkup data. These will be utilized in services such as regional healthcare enterprises [4]. In moving towards the implementation of EHRs and PHRs for managing and utilizing such medical and healthcare information, it is essential to conform to standardization and ensure interoperability, and activities to those ends are being performed vigorously. Once EHRs and PHRs have been implemented, it will be possible to configure an environment in which information can be utilized far more significantly, which should have a huge effect on problems such as rapidly rising medical expenses and medical quality. NTT research laboratories utilize ICT in the medical and health fields and are responding towards technology development and standardization intended to implement an even better society for our customers. References
|
|||||||||||||||||||||